This curated collection points family doctors to a careful selection of highly relevant resources to aid in better understanding Adverse Childhood Experiences (ACEs) and implementing Trauma-Informed, Resilience-Oriented Healthcare (TIROH). It derives from a CAFP family physician survey of information gaps and needs. Contact cafp@familydocs.org to suggest additional resources of value.
Introduction & Definitions
What Are Adverse Childhood Experiences (ACEs)?
Adverse Childhood Experiences (ACEs) are potentially traumatic events that occur when we are young. The term “ACEs” refers to 10 categories of adversities in three domains experienced by 18 years of age that were identified in the landmark 1998 study by the Centers for Disease Control and Prevention (CDC) and Kaiser Permanente. ACEs and the associated toxic stress they create are the root causes of some of the most common, serious, and costly health and social challenges facing our state.
What Is Trauma-Informed Resilience Oriented Healthcare (TIROH)?
Trauma-informed care shifts the focus from “What’s wrong with you?” to “What happened to you?” A trauma-informed approach to care acknowledges that health care organizations and care teams need to have a complete picture of a patient’s life situation — past and present — in order to provide effective health care services with a healing orientation.
TIROH is a framework of trauma-informed care that broadens the trauma-informed perspective beyond the patient experience to the entire organization. It is an organizational culture, structure and treatment framework built on understanding, recognizing and responding to trauma and toxic stress in patients AND staff. The TIROH framework enables individuals, organizations, communities and systems to shift their perspective and organizational culture in order to create safe, compassionate and equitable spaces that support resilience and minimize re-traumatization.
Adopting trauma-informed practices can potentially improve patient engagement, treatment adherence, and health outcomes, as well as provider and staff wellness. It can also help reduce avoidable care and excess costs for both the health care and social service sectors. (Trauma Informed Care Implementation Resource Center)
What Is Resiliency?
Resiliency is the ability to adapt to or recover from adverse events and stressors resulting from a combination of intrinsic factors (such as self-regulation or telomere length), extrinsic factors (like safe, stable, and nurturing relationships with family members and others), and predisposing biological susceptibility (Roadmap for Resilience: The California Surgeon General’s Report on Adverse Childhood Experiences, Toxic Stress, and Health, 2020).
What to Do?
When it comes to ACEs & TIROH, there is no single, perfect approach. There is a wide range of activities that can contribute to improved patient care. Consider your patient population and your practice environment as you integrate new practices.
Allow the following five recommendations guide you:
- An ACEs score is not a diagnosis. Like the ASCVD score estimates risk of a cardiovascular event, an ACEs score helps understand a patient’s risk of developing toxic stress. Not all patients with a high ASCVD score will have a heart attack. Similarly, not all patients with a high ACEs score will develop toxic stress and its sequelae. However, both scores could influence the conversations and care you have with your patient.
- Above all, the ACEs score is information for you and for your patient. Allow your patient to decide what their ACEs score means and what – if anything – to do with it.
- Focus on education rather than the number.
- Approach all patients through a TIROH lens, regardless of their ACEs score.
- Look inward to consider ACEs & TIROH for all staff and providers in your practice.
TIROH in Practice
There is a spectrum of TIROH practice, anywhere from using TIROH approaches in patient care all the way up to universal ACEs screening. Allow the following examples of TIROH in practice to guide and inspire you as you develop approaches best suited to your environment.
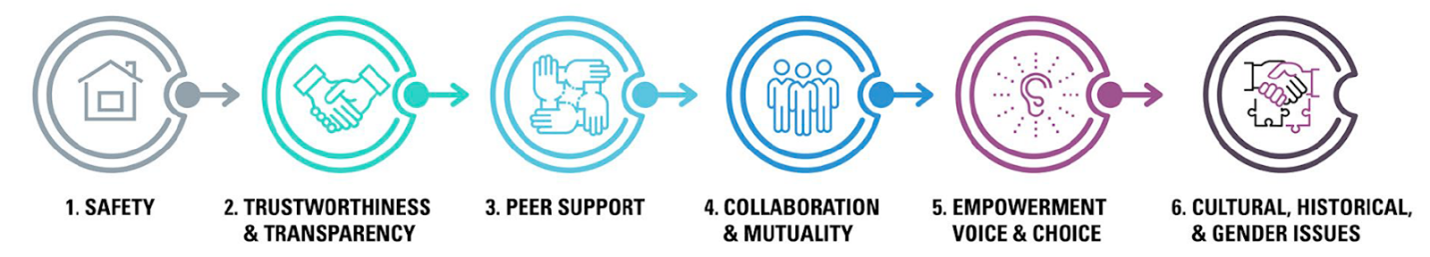
SAMHSA’s National Center for Trauma-Informed Care describes six principles that guide a trauma-informed approach. TIROH requires constant attention, caring awareness, sensitivity, and possibly a cultural change at an organizational level. On-going internal organizational assessment and quality improvement, as well as engagement with community stakeholders, will help to imbed this approach which can be augmented with organizational development and practice improvement.
The following links are examples of TIROH in practice:
Implementing Trauma Informed Tips in Your Environment
This seven-workshop series from Origins Training may be delivered by a local champion to introduce or reinforce a trauma-informed lens in your organization. Each workshop in the series is organized around a trauma-informed principle and offers three practical tips for bringing that principle to life. The materials include:
Facilitator Support for Series:
- Facilitator Guide, Slide Deck, and Video to support facilitators on how to implement the series. These include overview, general facilitator tips, and ideas for engaging participants in discussions and activities.
- Handout on understanding stress, trauma, and resilience to support a shared language.
Workshop Materials for Each Trauma Informed Tip: Slides contain facilitator notes & additional resources. Sample email texts are provided to share with participants after workshops to reinforce tips.
- Tips for Creating Safety - Slides & Email
- Tips for Trustworthiness & Transparency - Slides & Email
- Tips for Peer Support - Slides & Email
- Tips for Collaboration & Mutuality - Slides & Email
- Tips for Empowerment, Voice & Choice - Slides & Email
- Tips for Strengths-Based - Slides & Email
- Tips for Cultural, Historical & Gender Humility - Slides & Email
Clinical Resources
We encourage family physicians to complete the ACEs Aware Training for Screening (see below), while also holding the idea that ACEs may be relevant to all patients and remembering that the ACEs number is not a diagnosis that requires a specific treatment. Below you will find resources for screening, patient education, resilience information and suggested clinical workflows. The ACEs Aware Clinical Team Toolkit: Preventing, Screening, and Responding to the Impact of ACEs and Toxic Stress offers clinicians and practices comprehensive information and resources. This Toolkit is composed of a series of fact sheets that are designed to be read individually
Screening
- ACEs Aware Training for Screening The Becoming ACEs Aware in California training is a free, two-hour core training to learn about ACEs, toxic stress, screening, risk assessment, and evidence-based care to effectively intervene. The training is available to anyone. Clinical providers also can submit a DHCS Training Attestation form after completion of this training, so that they can bill Medi-Cal for screenings.
- Screening Tools Screening for ACEs helps primary care clinicians assess risk for toxic stress and guide effective responses. To receive Medi-Cal payment for conducting ACE screenings, clinical team members in California must use the following screening tools for children, adolescents, and adults. The tools are available in 17 languages and in de-identified and identified formats. Includes:
- Pediatric ACEs and Related Life-events Screener (PEARLS)
- ACE Questionnaire for Adults
-
- CAFP ACEs Screening FAQ A set of common and practical questions and answers about ACEs screening assembled from family physicians participating in the 2021 CAFP FIT (Family Medicine Initiative on Trauma-Informed Care) Initiative.
Patient Education
Resiliency
In brief, resiliency is the ability to adapt to or recover from stress. For a more complete definition, see the glossary of the 2020 Roadmap for Resilience, referenced below. The following are resources that help identify key factors to support resiliency.
- Stress Busters: Seven Ways to Manage Stress (ACEs Aware) Website, videos, handouts, additional resources, presented individually for each of the following topics: supportive relationships, quality sleep, balanced nutrition, physical activity, mindfulness practices, experiencing nature, and mental healthcare.
- Adverse Childhood Experiences Prevention: Resource for Action (CDC) This is a resource to help states and communities leverage the best available evidence to prevent ACEs from happening in the first place as well as lessen harms when ACEs do occur. It features six strategies drawn from the CDC Resources for Action, formerly known as, “technical packages.”
- Roadmap for Resilience: The California Surgeon General’s Report on Adverse Childhood Experiences, Toxic Stress, and Health (CA OSG) A foundational 2020 report from Nadine Burke Harris and others. Describes California’s approach and includes primary, secondary and tertiary prevention strategies in healthcare, public health, social services and more. Also includes clinical implementation case studies.
- Numberstory.org, Spanish (ACE Resource Network) An inspiring and accessible multimedia journey explaining ACEs and providing a large collection of resources for patients and healing professionals.
Workflows
Links below are suggested as starting points for your own, unique process that will reflect your particular population and practice environment.
Justice, Equity, Diversity & Inclusion
Justice, equity, diversity and inclusion (JEDI) is central to CAFP’s strategic plan and is part of everything that we do. In the case of ACEs, JEDI awareness is mandatory in order to create a genuinely trauma-informed healing environment.
Regional Resources
Help us make this resource stronger by sending regional resources to cafp@familydocs.org.
- Neighborhood Navigator (AAFP EveryONE Project) Use this interactive tool at the point of care to connect patients with supportive resources in their neighborhoods. It lists more than 40,000 social services by zip code: food, housing, transportation, employment aid, legal aid, financial assistance.
- One Degree Life-improving resources in Los Angeles County and the San Francisco Bay Area
- Yolo County Health Resource Center Information on health, childcare, transportation, food, and other resources in Yolo County.
- Find a Meeting
Key Organizations
Organizations here represent a California-centric sample of those committed to the work of healing and resilience for those affected by adverse childhood experiences.
- California Academy of Family Physicians CAFP empowers, educates, and connects current and future family physicians to improve the health of all. CAFP’s strategic plan goal of prioritizing Justice through Diversity, Equity and Inclusion (JEDI) necessitates attention to ACEs and TIROH.
- ACEs Aware - ACEs Aware strives to create a better world for our children, families, and communities by working together across sectors to prevent and address the impact of ACEs and toxic stress. ACEs Aware is a state-wide initiative led by the Office of the California Surgeon General and the Department of Health Care Services, implemented by the UCLA/UCSF ACEs Aware Family Resilience Network (UCAAN), to screen children and adults for Adverse Childhood Experiences (ACEs) in primary care, and to treat the impacts of toxic stress with trauma-informed care. It includes giving Medi-Cal providers training, clinical protocols, and payment for screening children and adults for ACEs.
- ACEs Aware Resources - A large and well-organized collection of clinical resources, organizational toolkits, family handouts, and policy, research and advocacy briefs.
- Center on the Developing Child (Harvard) The mission of the Center on the Developing Child is to drive science-based innovation that achieves breakthrough outcomes for children facing adversity. The Center catalyzes local, national, and international innovation in policy and practice focused on children and families. We design, test, and implement these ideas in collaboration with a broad network of research, practice, policy, community, and philanthropic leaders. Together, we seek transformational impacts on lifelong learning, behavior, and both physical and mental health.
- Office of the California Surgeon General Advancing systemic reforms that recognize and respond to the effects of ACEs on lifelong health – all driven by equity. With DHCS, started ACEs Aware. A 2023 public awareness campaign aims to give youth and young adults across California the resources and strategies they need to manage stress, heal from adversity, and end cycles of trauma.
- PACEs Connection PACEs Connection, an ever-growing social network, connects those who are implementing trauma-informed and resilience-building practices based on ACEs science. The network’s 40,000+ members share their best practices, while inspiring each other to grow the PACEs movement.
- Positive Discipline – Dr. Jane Nelson Resources for parents, teachers and counselors to teach social and life skills through encouragement and mutual respect for every life stage. Books, online learning, apps and more.
- Trauma-Informed Care Implementation Resource Center - Curates resources from experts in the field of trauma-informed care across the country and also draws largely from the experiences of health care organizations that participated in Advancing Trauma-Informed Care. This multi-site demonstration, led by the Center for Health Care Strategies and made possible through support from the Robert Wood Johnson Foundation, sought to identify how trauma-informed approaches can be practically implemented across the health care sector.